Version 4.1.10
|
|
OneView Physician Quality Release Notes
What's New in OneView Physician Quality 4.1.10
Release Date: Wednesday, October 11, 2017
Overview introduction help guide of OneView 4.1.10 Release including manage dictionaries, validation reports, and MIPS dashboard.
New Features and Enhancements:
Manage Dictionaries:
- CPOE OE Categories updated header label to be consistent on the form.
- Updated dictionary code for additional fields for ACI, OM, and IA measures to be selected in dictionary.
Reports:
- ACI Reports/MIPS Dashboard:
- The reports and MIPS dashboard have been updated to check for base measures requirements, checking for at least 1 patient for HIE and PEA measures, and 1 prescription for EP measure.
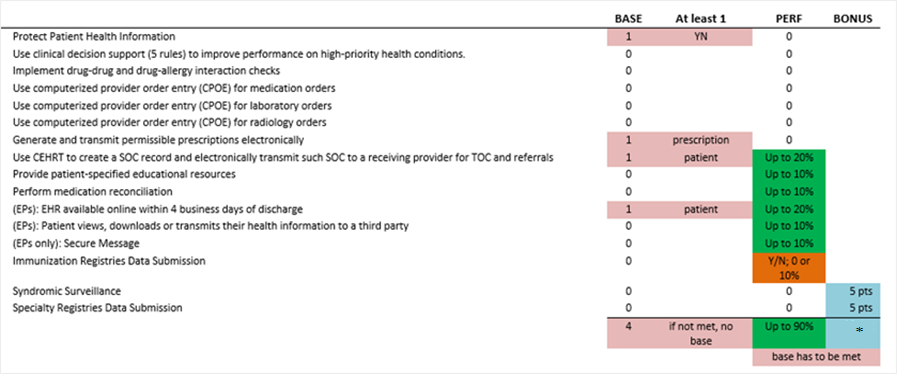
* Report to one or more additional public health and clinical data registries beyond the Immunization Registry Reporting measures to get 5% bonus.
- The reports and MIPS dashboard have been updated to include Public Health and Clinical Data Registry reporting measures as individual measures instead of grouping them together so we can now incorporate them individually in the bonus calculation for MIPS.
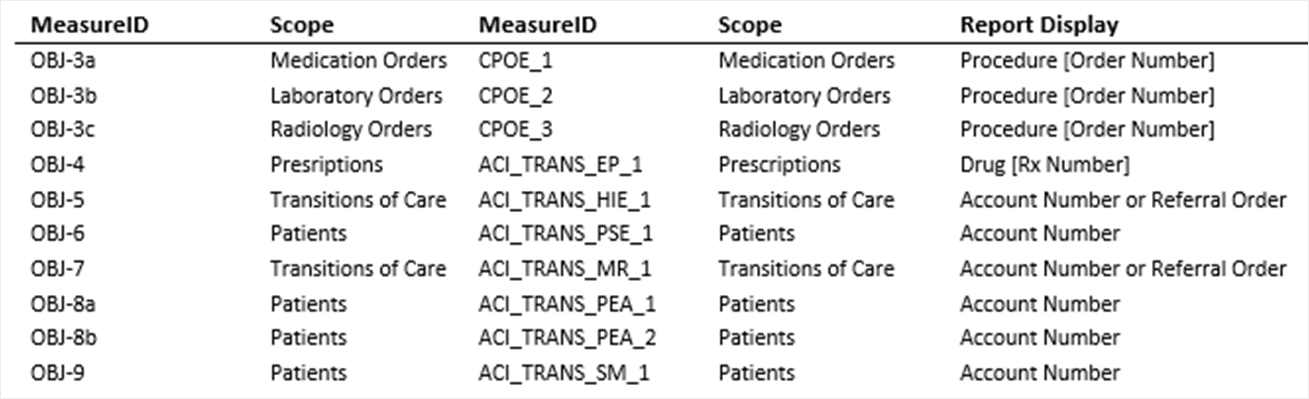
- Updated the Report Display wording for Patient and TOC measures.
- Report Update: Added list of providers to the CQM Group report, so that you can see the providers in that group (for groups not using the group reporting option).
- Updated ACI reports to include Scope information on the detailed Patient Yes/No Report.
- Updated ACI Summary and By Group to show calculation criteria for points, using base measures, and minimum requirements met for base measures.
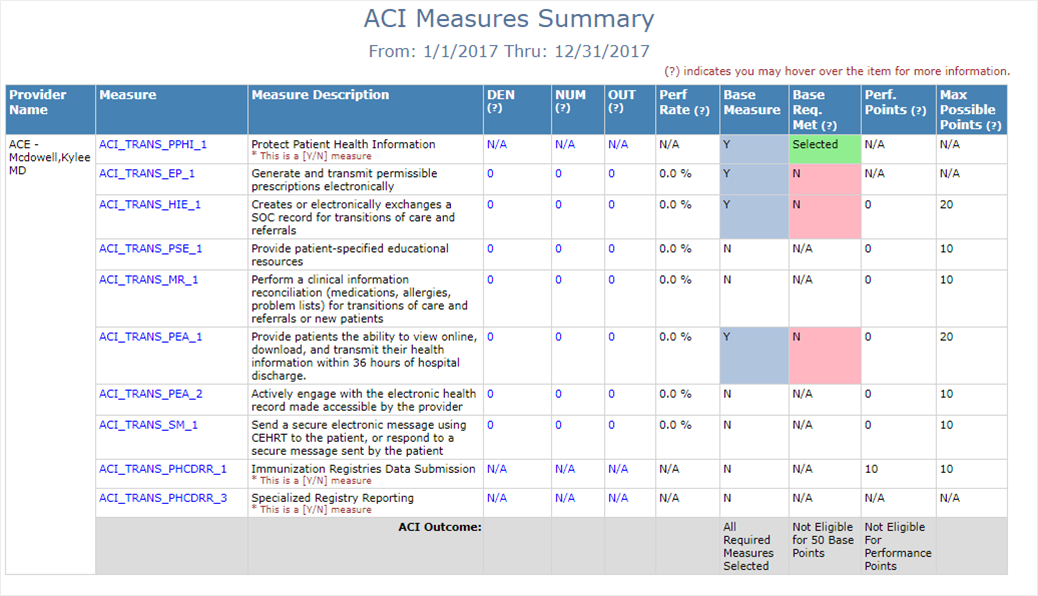
- Enhanced performance when returning the ACI circle on dashboard.
- Updated MIPS dashboard to limited groups and providers only participating in the QPP MIPS submission programs. For Groups, they will only display on dashboard if the Group Reporting check box is selected.
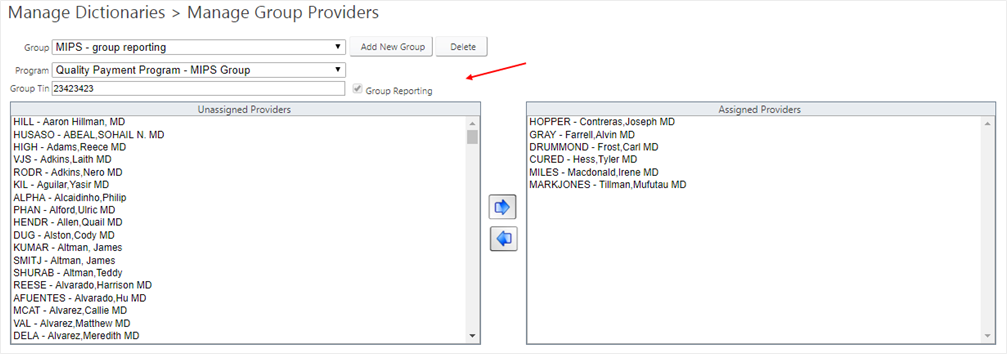
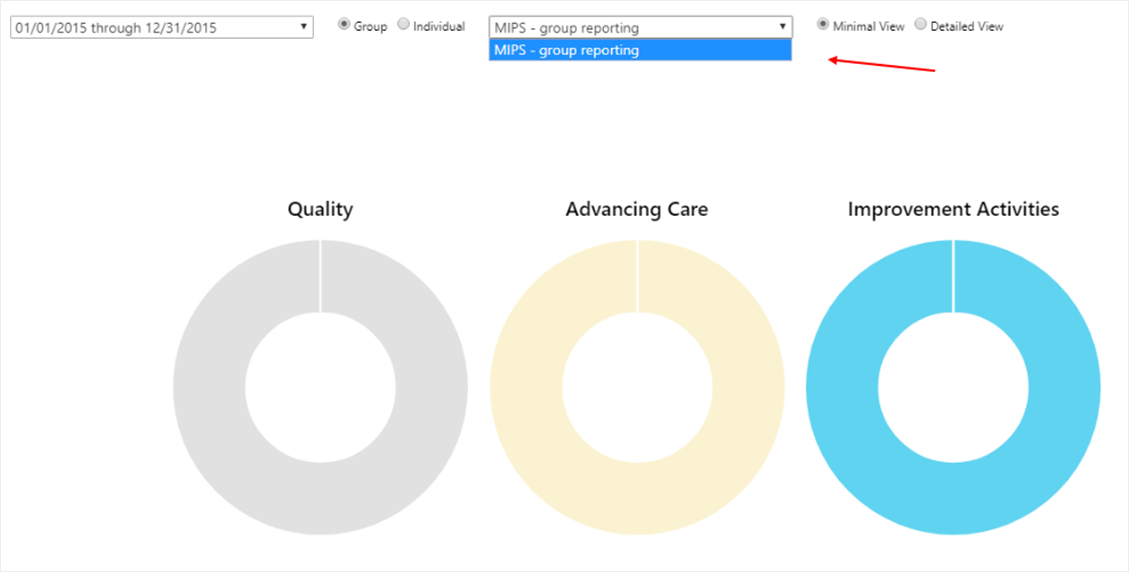
- For more helpful information on the MIPS Dashboard and Reports, please read the introduction help guide for OneView 4.1.10.
- Clinical Quality Measures:
- Removed measurement period as a valid value set to be mapped in the report.
- Added list of providers to the CQM Group report, so that you can see the providers in that group (for groups not using the Group Reporting option).
Advancing Care Information:
- Improved performance for RxmRxs data compile.
- Updates to the scope logic for denominator calculations for Acute Care services.
- Add Index to improve measure compile
Clinical Quality Measures:
- Enhancements to the calculation engine performance.
- Updates to the population collection to include sex, age, DOB, and race in the patient population.
- Updated the value set for the Gender for CQMs to determine Male/Female for certain specs.
Fixes:
Manage Dictionaries:
- Updates to settings for handling MAT and MAT60 versions in app settings.
- Updates to the provider dictionary to help remove providers that shouldn't be in the list.
- CPOE OE Categories updated header label to be consistent on the form.
Reports:
- Corrected score calculations for Dashboard; related to the bonus for PHR measures.
Advancing Care Information:
- Corrected bug for data coming from AbstractData that was not associated with a specific account number.
- Updates to the initial population to include location and Unit Number.
- Updates to the measure collection for eRX.
- Add Monograph Availability to Patient Education
- Magic - Fixed bug in join to nursing interventions table
- Add Education Resources to data collection for VDT
- Add SourceID to join matching for RegAcctQuery_Result
- Fix incorrect join when populating order table
- Reorder column populate of DataRxmRxDetails in Magic
Clinical Quality Measures:
- Magic only - Corrected bug in immunization code to pull patient id from PBR.
- Client Server only - Made improvements to family history code to improve performance
- Improved medication dosing days logic to prevent arithmetic overflow of the datatype and avoid dividing by zero.

